Berkeley
After Brazil Olympics, Zika Continues to Plague Babies in Urban Slums

Arts and Culture
Farwest Region Deltas Celebrate Centennial With “September Breakfast” Honoring Vivian Osborne Marsh
The region was established in 1925 under the leadership of Vivian Osborne Marsh, who became its first Regional Director. Marsh was a pioneering scholar and civic leader, earning recognition as the first Black woman to receive both a bachelor’s and a master’s degree in anthropology from UC Berkeley.

Arts and Culture
Cal Performances Presents Angélique Kidjo & Yo-Yo Ma in Sarabande Africaine at UC Berkeley Greek Theatre on Aug. 30
On Saturday, Aug. 30, the pair will debut the Bay Area premiere of Sarabande Africaine, joined by pianist Thierry Vaton, percussionist David Donatien, and special guest Sinkane. The program illuminates centuries of musical interplay between African traditions and Western classical forms, using the Baroque sarabande dance, and its African ancestor, the Congolese spirit dance Zarabanda, as a gateway to exploring the deep, interconnected roots of global music.
Activism
The Case Against Probate: False Ruling Invalidates Black Professor’s Estate Plan, Ignoring 28-Year Relationship
Zakiya Folami Jendayi, beneficiary of Head’s estate, states that “The errors, ranging from misstatements of fact, omissions of critical evidence, and reliance on false arguments and testimony, formed the basis of Judge Sandra K. Bean’s ruling against me, Dr. Head’s previous student, mentee, sorority sister and long-time friend,and despite the fact that I was her chosen, power of attorney, Advanced Healthcare Directive agent, trustee, executor and sole beneficiary.”

-

 Advice3 weeks ago
Advice3 weeks agoBook Review: Books for College-Bound Students
-

 Arts and Culture4 weeks ago
Arts and Culture4 weeks agoAgainst All Odds: Mary Jackson’s Journey to NASA Engineer
-

 Bay Area3 weeks ago
Bay Area3 weeks agoQ&A with Steven Bradford: Why He Wants Your Vote for California Insurance Commissioner
-

 Activism3 weeks ago
Activism3 weeks agoOPINION: The Fire of Oakland’s Justin Jones
-

 Alameda County4 weeks ago
Alameda County4 weeks agoThe Marin City Flea Market Is Back
-
 Activism3 weeks ago
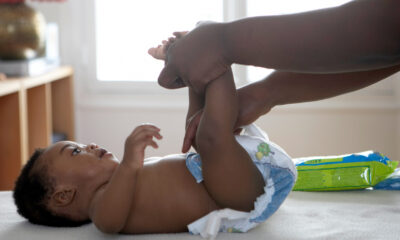
Activism3 weeks agoCalifornia Launches Free Diaper Program for Newborns Statewide
-

 Activism3 weeks ago
Activism3 weeks agoThe Ladies of Delta Sigma Theta Hold Day of Advocacy at the Capitol in Sacramento
-

 Activism4 weeks ago
Activism4 weeks agoEBMUD Enshrines the Legacy of its First Black Board Member William ‘Bill’ Patterson




















































